Healthcare Quarterly
Advancing Integrated Care: Harnessing Research, Knowledge Mobilization and Collective Impact as Levers of Transformation
Meghan McMahon*, Jessica Nadigel*, Bahar Kasaai, Nida Shahid, Rhonda Boateng and Richard H. Glazier
Abstract
Canada has faced criticism as being a land of pilot projects with an implementation crisis in healthcare. This paper explores the power and promise of research to serve as a strategic lever for advancing integrated care implementation and impact across Canada. It examines the evolution of the Canadian Institutes of Health Research's approach to funding integrated care research and promoting its uptake over time. Through case studies and analysis of funding trends, capacity generated and impacts achieved, the paper illustrates how coordinated integrated care research investment can support evidence-informed integrated care transformation.
Introduction
The International Foundation for Integrated Care (IFIC) Canada has issued a bold and essential call to transform care through integration (Wojtak and Lewanczuk 2025). Transformation is required to shift from our current landscape of siloed sectors and services, fragmented care pathways, inequitable access and outcomes and a sickness-oriented model, to an integrated system that enhances population health and well-being for all. Such transformation requires a range of coordinated actions and inputs, including clear vision, effective leadership, cross-sector collaboration, refreshed governance and accountability structures, aligned incentives and funding and a relentless commitment to continuous improvement. Achieving this at scale and with sustained impact also demands a robust evidence base to inform potential solutions, guide their implementation, rigorously evaluate what works for whom and under what conditions and support the spread and scale of those solutions that demonstrate promise.
Research evidence is often criticized for being irrelevant to real-world needs and slow to translate into practice (Graham et al. 2006; Morris et al. 2011). Canada has had difficulty shaking its reputation as a “country of perpetual pilot projects” (Bégin et al. 2009), which Bégin et al. posit “began in 1975 … when Health Canada launched the National Health Research and Development Program (NHRDP)” (Bégin et al. 2009). More recently, the country also faced criticism for having an “implementation crisis” (Picard 2023).
The production and translation of evidence into action is precisely the role of the NHRDP's successor, the Canadian Institutes of Health Research (CIHR). CIHR has a legislated mandate to create new knowledge and translate it into improved health for Canadians, more effective health services and products and a strengthened Canadian healthcare system (CIHR 2000). CIHR applies its mandate and its funding, convening and partnering levers to generate evidence and mobilize it into action in key priority areas. Integrated care has been a longstanding health system priority and a CIHR focus for research investment, partnership and action.
This paper explores the power and promise of research to serve as a strategic lever for advancing integrated care across Canada. It examines the evolution of CIHR's approach to funding integrated care research and promoting its uptake into policy and practice over a 25-year period, from 2000 to 2025. Drawing on analyses of funding trends and case studies of research impact, this paper outlines lessons applicable to system leaders across jurisdictions aiming to use research to advance integrated care transformation.
A Persistent Priority Through Time With Evolution in Research Funding Strategies
A broad approach to research priorities and investments: Listening for Direction (2001–2007)
As shown in Table 1 (available online here), integrated care has featured in foundational research prioritization documents since the beginning of CIHR. In 2001, the national priority-setting initiative led by the Canadian Health Services Research Foundation (now Healthcare Excellence Canada), Listening for Direction (LfD), identified the “continuum of care and delivery models” as a priority research theme for investment and action (Gagnon and Menard 2001). In 2004, the initiative was repeated and LfD II featured integrated care in two of the prioritized research themes: “linking care across place, time and settings” and “linking public health to health services” (Dault et al. 2004). A third refresh in 2007 featured integrated care as a “Patient Flow and System Integration” priority (Law et al. 2008).
The LfD exercises aimed to coordinate priority-setting across national organizations to reduce duplication, identify shared priorities and foster collaborative partnerships. Although CIHR's Institute of Health Services and Policy Research (IHSPR) adopted the LfD priorities in its early-year strategic plans and as relevant research areas within its funding programs, it did not make targeted investments to advance integrated care. IHSPR's broad adoption of LfD priorities reflects both the nascent state of the health services and policy research (HSPR) community at that time and the institute's role in galvanizing a community with the capacity to tackle a range of health system priorities.
A targeted approach to integrated care-related research priorities and investments: community-based primary health care (2010–2018)
Beginning in 2010, IHSPR adopted a more targeted approach to priorities and investments. The institute launched large-scale strategic initiatives focused on integrated care-related priorities, beginning with the Community-Based Primary Health Care (CBPHC) signature initiative (CIHR n.d.d). This initiative reflected the policy, practice, patient and research priorities identified through pan-Canadian engagement, which revealed a consensus that traditional primary care models were outdated and ill-equipped to meet increasing levels of complexity and multimorbidity. IHSPR and the Institute of Population and Public Health, with Canadian and international partners, created and launched the CBPHC initiative. CBPHC comprised a suite of strategic research programs that included innovation teams, embedded clinician scientists and new investigators, a network and several other strategic programs (Table 1), all with a shared aim to improve the delivery of high-quality CBPHC to Canadians. Absent from the initiative design was a central coordinating hub to foster sharing and learning across funded grantees and to mobilize findings into action. Still, the initiative generated new evidence on CBPHC models, built cross-provincial capacity in primary care research and international collaborations and sparked the spread and scale of evidence into action (see below).
Embracing Transitions in Care (2018 – onward)
In 2018, IHSPR widened its integrated care focus to take a sector-agnostic approach centred on transitions in care. Through co-leadership with CIHR institutes (CIHR's Institute of Circulatory and Respiratory Health, Institute of Human Development, Child and Youth Health and Institute of Indigenous Peoples' Health) and partnerships within and external to CIHR, the Transitions in Care initiative was launched (CIHR n.d.f). This initiative recognized that Canada's health systems are organized in a way that requires individuals to navigate multiple transition points where vulnerabilities can arise. IHSPR and its partners collaboratively designed and launched a series of interrelated funding opportunities to address transitions in care knowledge gaps with actionable evidence (Table 1). Similar to the CBPHC initiative, the Transitions in Care initiative design lacked a coordinating hub to support cross-project learning, aggregate key insights and mobilize evidence into action. The initiative is presently in progress with early outcomes and impacts showing promise (CIHR 2025).
Prioritizing implementation and transformation: Transforming Health with Integrated Care (2021 onward)
Integrated care has remained a top priority. Throughout IHSPR's 2021 pan-Canadian listening tour to inform its strategic plan, integrated care was consistently identified by policy makers, healthcare providers, patients and researchers across Canada as a critical area of focus (McMahon et al. 2022), albeit with an important shift in the type of research needed. Instead of calls for the development of new integrated care models and solutions (the “what”), emphasis was on supporting the implementation (the “how”) of proven solutions into practice. This emphasis underpinned the design of IHSPR's Transforming Health with Integrated Care (THINC) initiative (CIHR n.d.h).
Launched in 2023 by IHSPR and 12 federal and provincial partners through an evidence-informed, community-engaged approach (described by Shahid et al. 2025), THINC aims to advance knowledge on how to implement, evaluate and spread and scale evidence-informed integrated care solutions that advance the Quintuple Aim (CIHR-IHSPR 2023). THINC represents an evolution and maturation in the research funding strategies and design elements used to advance transformative impact.
THINC comprises two flagship components: five-year implementation science teams (ISTs) and a six-year Knowledge Mobilization (KM) and Impact Hub. It also comprises embedded researchers and one-year catalyst grant programs grounded in policy relevance, co-design and advancement of the Quintuple Aim (Table 1).
To move beyond Canada's “pilot project” and “implementation crisis” paradigms toward implementation and impact, the THINC ISTs require a focus on “transformative evidence-informed integrated care policies and intervention(s) that have … evidence of effectiveness and/or promising results on improved integration of services and improved outcomes” (CIHR 2023; Shahid et al. 2025). In addition, to enhance relevance, reach and impact, all ISTs have: a core focus on implementation science; a quadripartite shared team leadership (involving research, policy, provider and patient experience); a commitment to large-scale, system-level transformation involving multiple organizations, jurisdictions and sectors; clear impact goal(s) grounded in the Quintuple Aim; and a dedicated KM and Impact Champion that liaises with the Hub.
THINC with collective impact
THINC's flagship KM and Impact Hub, called the Network for Integrated Care Excellence (NICE), has a mandate to “build and support a vibrant pan-Canadian learning community involving all THINC grantees and knowledge user communities toward advancing evidence-informed integrated care transformation and catalyze progress toward achieving the Quintuple Aim” (CIHR 2023). The NICE Hub creates connections across the THINC grantees, system leaders, providers, community members and people with lived/living experience (PWLE). It fosters collaboration, capacity and shared practices across sectors, organizations and people while advancing a common goal of evidence-informed integrated care transformation. It promotes shared learning internationally through its co-location within the North American Centre on Integrated Care and its relationship with IFIC. THINC shares IFIC Canada's aspiration to transform care through integration and is viewed as playing a crucial role in enabling and amplifying integrated care research impact.
What Worked? Evidence of Impact
Integrated care funding trends and capacity over time
Integrated care was a consistent research priority over the last 25 years, though the focus evolved from CBPHC to transitions in care, to transformative integrated care systems. The research funding strategies used to advance integrated care also evolved from a broad approach of including integrated care as one of many relevant research areas in funding calls, to a targeted approach of designing large-scale, partnered, multi-component strategic initiatives, to the current impact-oriented approach grounded in implementation science with a dedicated collective impact hub.
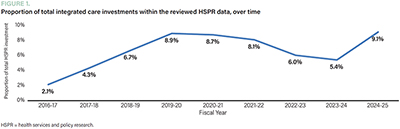
Concurrent with this evolution in funding strategy, the share of integrated care research investment within CIHR's HSPR funding has evolved over time from 2.1 to 9.1% over the nine-year period from 2016–2017 to 2024–2025 (Figure 1). The size of the integrated care research community has also changed over the same time frame, as shown in Figure 2. The size is projected to increase with the infusion of THINC-related investment.
Realizing impacts: spotlight on the CBPHC signature initiative
Within these initiatives and data trends are stories of research impact. Evaluations of final grant reports show evidence of knowledge creation, capacity development, evidence-informed decision-making and contributions to enhanced health and health system performance. Table 2 summarizes the research impacts achieved by the CBPHC Innovation Teams and Embedded Clinician Researcher Awardees (CIHR 2022a, 2022b, 2022c; Wong et al. 2019).
| TABLE 2. CBPHC research impacts | ||
| Impact Category* | CBPHC Innovation Teams | ECRAs |
| Knowledge creation | 300+ publications Development of common indicators measured across all teams (Wong et al. 2019) |
165 publications Two intellectual properties (patents) |
| Capacity building | 300+ trainees and 95 postdoctoral researchers mentored | Trained and mentored 184 trainees and 86 research staff |
| Informing decision making | 56 policy briefs and guidelines developed 80 media engagements Partnered with almost 200 policy makers, 1,000 healthcare providers and 40 patient and community members |
118 media engagements Partnered with 20 health system partner organizations |
| Engaged more than 230 healthcare providers, policy makers and patient and community partners 42+ invited presentations delivered to policy makers and other knowledge users |
||
| Enhancing health system performance | Developed, scaled and spread more than 31 models of CBPHC in 11 Canadian jurisdictions and six countries, and with reported positive impacts on equity-denied and rights-holding populations | 44+ interventions implemented, tested and spread and scaled across Canada |
| CBPHC = community-based primary health care; ECRA = Embedded Clinician Researcher Award. | ||
One example of improved health system performance through scale and spread comes from the “Advancing primary healthcare for persons living with HIV in Canada” CBPHC innovation team led by Clare Liddy and Claire Kendall (CIHR 2021). This team aimed to close gaps in the continuum of care through the use of digital health solutions. Their grant supported the Champlain Building Access to Specialists through eConsultation (BASE) eConsult service, a secure online platform that allows primary care providers and specialists to communicate regarding a patient's care. Demonstrating reduced wait times for specialist care, savings to patients from avoidance of travel-associated costs and high patient and provider satisfaction, the service spread across Ontario (Liddy et al. 2022) and beyond (Liddy et al. 2017; Singer et al. 2022) and is currently recognized as a world leader in eConsultation.
Additional research impact examples stem from the Embedded Clinician Researcher Award (ECRA) program, including Patrick Archambault's ECRA with Quebec's Centre intégré de santé et de services sociaux de Chaudière-Appalaches (CISSS-CA) and with Naana Afua Jumah's ECRA with the Thunder Bay Regional Health Sciences Centre (CIHR 2022d).
Archambault and team sought to implement, adapt and scale the Acute Care for Elders program with Geriatric Emergency Medicine nurses in four hospitals in the CISSS-CA. The evidence-based intervention focused on improving the transitions of frail seniors from emergency departments to the community. Through measurement of the intervention's impact on patient, caregiver, clinical and hospital outcomes, and assessment of the underlying mechanisms for local adaptation, their research supported the intervention's spread to additional hospitals in the region (IHSPR 2022a).
Jumah and team addressed the fragmented perinatal care in Northwestern Ontario. Using the Truth and Reconciliation Commission of Canada Calls to Action as the guiding framework, they partnered with a dozen Indigenous women's organizations and Thunder Bay Regional Health to develop, test and implement interventions to improve perinatal care. Their Hearing Our Voices intervention (https://nurture-north.org/hearing-our-voices-an-indigenous-womens-reproductive-health-curriculum) – an online provider training program to learn about the social determinants of Indigenous women's health and how to deliver more culturally appropriate care – spread beyond the region following demonstrated success to achieve national uptake involving 500 participants. Their Maternal Infant Support Worker Program (https://nurture-north.org/maternal-infant-support-worker-misw-program-evaluation) trained 11 local women living in remote First Nations to provide lay perinatal care and mental wellness training, leading to better perinatal care for women closer to home and spurring increased interest in Indigenous midwifery in the region (IHSPR 2022b).
Facilitators and barriers to research impact
The CBPHC Innovation Teams and ECRAs shared similar facilitators and barriers to the spread and scale of interventions. Successful efforts were driven by robust partnerships and early engagement with policy and decision makers and PWLE, ensuring that interventions aligned with priority needs. Interdisciplinary teams, collaborative leadership and effective communication fostered strong collaboration across the teams and their partners. In addition, the growing adoption of digital health over the time period of the initiative facilitated intervention implementation and uptake. However, the spread and scale were hindered by shifting political environments, fragmented and non-interoperable data structures and contextual challenges such as personnel turnover, resistance to change and the slow pace of evidence adoption (CIHR 2022b, 2022c).
THINC-ing toward the future
The THINC initiative is currently in its second half of a six-year funding term and is already showing evidence of impact. The NICE Hub is a radical new approach to funding KM and research impact. Instead of situating these responsibilities solely within individual and potentially siloed research teams, The Hub recognizes the criticality of collective impact approaches. It provides the backbone infrastructure and intellectual leadership to build community across teams, to connect them to national and international integrated care networks and to advance their collective contribution to integrated care transformation. For example, The Hub's launch of “learning communities” was designed to create sustained connections across teams and to share and learn from each other's experiences. On the international front, The Hub and IHSPR co-hosted a workshop at the 2024 and 2025 IFIC conferences to spark global conversations around shared integrated care challenges and opportunities. Looking ahead, The Hub will deepen its relationships with policy and decision makers, strengthen the teams' connections with national and international integrated care networks and begin to aggregate learnings across teams, mobilize evidence into action and support the scale and spread of the teams' innovation successes.
Going forward, IHSPR will continue to support KM and impact assessment of research initiatives such as THINC to maximize the value that research yields for integrated care transformation. By drawing on made-in-Canada research impact assessment frameworks (CHSPRA 2018) and exemplars of impact assessment of large-scale HSPR funding initiatives (Nadigel et al. 2025), IHSPR will embed continuous learning and improvement within its funding strategies.
Lessons Learned and Implications for System Leaders
Over the past 25 years, integrated care research has been a sustained priority for investment, yielding a substantial record of impact. Although the specific areas of focus have evolved and the funding strategies have matured, research investment has consistently enabled improvements in integrated care.
This story of integrated care research investment and impact illustrates for system leaders the value of research as a lever for improvement and transformation. Research can support integrated care delivery teams and system leaders advance toward their goals with success, generate data-driven insights to improve the implementation and outcomes of integrated care interventions, provide real-time information on whether an intervention is achieving its intended effect (and adapt and improve it if not) and improve the sustainability and long-term benefits of integrated care. In an era of fiscal constraint, competing priorities and a desire to build prosperity for all, system leaders should be assured by the value proposition for integrated care research.
To fully realize this value proposition, system leaders are invited and encouraged to engage with research. There are several concrete ways to do so. First, system leaders can help shape research priorities by engaging with funders such as CIHR and IHSPR in strategic planning exercises to share their evidence needs and gaps. This helps to ensure that strategic investments, such as CBPHC and THINC, are grounded in real-world evidence needs. Second, system leaders can support their teams and organizations to partner with researchers through opportunities similar to the innovation teams and others described throughout this paper, to help address complex challenges with the best available evidence. Third, system leaders can enhance their internal organizational capacity for research, rapid learning and continuous improvement by engaging in embedded research opportunities. Fourth, system leaders can leverage the findings from programs such as the THINC ISTs to identify which integrated care models work, for whom and under what conditions; anticipate contextual barriers; and scale successful models effectively across diverse settings. Finally, the NICE Hub serves as an exemplar of a central resource for system leaders to engage with research that addresses complex challenges, partner with researchers to generate solution-oriented evidence and join a collective movement to advance integrated care transformation across Canada.
Disclosures
The views expressed herein are solely those of the authors and do not necessarily reflect those of the Canadian Institutes of Health Research (CIHR).
About the Author(s)
Meghan McMahon, Phd, is an associate scientific director with the Canadian Institutes of Health Research (CIHR) Institute of Health Services and Policy Research and assistant professor with the Institute of Health Policy, Management and Evaluation at the University of Toronto in Toronto, ON. Meghan McMahon can be reached by e-mail at mmcmahon.ihspr@ices.on.ca.
Jessica Nadigel, Phd, is an associate scientific director with the CIHR Institute of Health Services and Policy Research in Toronto, ON.
Bahar Kasaai, Phd, is an assistant director with the CIHR Institute of Population and Public Health in Montreal, QC.
Nida Shahid, Phd, is a lead with the CIHR Institute of Health Services and Policy Research in Toronto, ON.
Rhonda Boateng, MSc, is a lead with the CIHR Institute of Health Services and Policy Research and doctoral candidate with the Institute of Health Policy, Management and Evaluation at the University of Toronto in Toronto, ON.
Richard H. Glazier, MD, MPH, is a scientific director with the CIHR Institute of Health Services and Policy Research, a senior core scientist with ICES and a staff family physician with St. Michael's Hospital, in Toronto, ON.
Acknowledgment
The authors gratefully acknowledge the invaluable contributions of the past scientific directors of the Canadian Institutes of Health Research (CIHR)-Institute of Health Services and Policy Research (IHSPR), Morris Barer, Colleen Flood and Robyn Tamblyn, whose vision and leadership laid the foundation for advancing integrated care research. The authors thank Erin Thompson, a former member of CIHR-IHSPR, for contributing toward developing integrated care impact stories. The authors wish to acknowledge and thank all the partners who helped design and shape the integrated care initiatives referenced in this article and the research community that is leading innovative, world-class, impact-oriented research.
References
Bégin, M., L. Eggertson and N. Macdonald. 2009. A Country of Perpetual Pilot Projects. CMAJ 180(12): 1185. doi:10.1503/cmaj.090808.
Canadian Health Services and Policy Research Alliance (CHSPRA) Impact Analysis Working Group. 2018, August. Making an Impact: A Shared Framework for Assessing the Impact of Health Services and Policy Research on Decision-Making. Retrieved January 16, 2026. <https://docs.wixstatic.com/ugd/5adc92_3ae941eaedb04ab4a66b6f83f98a479d.pdf?platform=hootsuite&mc_cid=47f94af269&mc_eid=ffbad33983>.
Canadian Institutes of Health Research (CIHR). 2000. Canadian Institutes of Health Research Act S.C. 2000, c. 6. Retrieved November 21, 2025. <https://laws-lois.justice.gc.ca/eng/acts/C-18.1/FullText.html>.
Canadian Institutes of Health Research (CIHR). 2021. Community-Based Primary Health Care Research Profiles. Retrieved November 23, 2025. <https://cihr-irsc.gc.ca/e/50370.html#it7>.
Canadian Institutes of Health Research (CIHR). 2022a. CBPHC Innovation Teams. Retrieved November 21, 2025. <https://cihr-irsc.gc.ca/e/52982.html>.
Canadian Institutes of Health Research (CIHR). 2022b. Community-Based Primary Health Care (CBPHC) 12 Innovation Teams: Summary of Innovative Models, Scale-Up, Knowledge Translation Products and More (From 2013 to 2019). Retrieved November 21, 2025. <https://cihr-irsc.gc.ca/e/52315.html>.
Canadian Institutes of Health Research (CIHR). 2022c. Embedded Clinician Salary Awards (ECRA): Executive Summary of Final Reports (May 2015 to April 2021). Retrieved November 21, 2025. <https://cihr-irsc.gc.ca/e/52980.html>.
Canadian Institutes of Health Research (CIHR). 2022d. Embedded Clinician Researcher Salary Awards. Retrieved November 21, 2025. <https://cihr-irsc.gc.ca/e/50368.html>.
Canadian Institutes of Health Research (CIHR). 2023. THINC Knowledge Mobilization & Impact Hub Funding Opportunity. Retrieved November 21, 2025. <https://www.researchnet-recherchenet.ca/rnr16/vwOpprtntyDtls.do?prog=3819&view=search&terms=hub&type=EXACT&resultCount=25&next=1>.
Canadian Institutes of Health Research (CIHR). 2025. What We Heard: Advancing Transitions in Care. Retrieved November 21, 2025. <https://cihr-irsc.gc.ca/e/54493.html>.
Canadian Institutes of Health Research (CIHR). n.d.a. Institute of Health Services and Policy Research Strategic Plan 2009–2014. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/41544.html>.
Canadian Institutes of Health Research (CIHR). n.d.b. CIHR Institute of Health Services and Policy Research Strategic Plan 2015-19. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/49711.html>.
Canadian Institutes of Health Research (CIHR). n.d.c. Canadian Institutes of Health Research – Institute of Health Services and Policy Research Strategic Plan 2021-2026. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/52481.html>.
Canadian Institutes of Health Research (CIHR). n.d.d. Community-Based Primary Health Care. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/43626.html>.
Canadian Institutes of Health Research (CIHR). n.d.e. Pan-Canadian SPOR Network in Primary and Integrated Health Care Innovations. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/49554.html>.
Canadian Institutes of Health Research (CIHR). n.d.f. Transitions in Care. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/50971.html>.
Canadian Institutes of Health Research (CIHR). n.d.g. Transforming Health With Integrated Care. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/52996.html>.
Canadian Institutes of Health Research (CIHR). n.d.h. Transforming Health With Integrated Care (THINC): Implementation Science Teams and Knowledge Mobilization and Impact Hub. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/53831.html>.
Canadian Institutes of Health Research (CIHR). n.d.i. End-of-Grant Policy Research Roundtable: Summary Report. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/54136.html>.
Canadian Institutes of Health Research (CIHR). n.d.j. The Health System Impact Program. Retrieved January 16, 2026. <https://cihr-irsc.gc.ca/e/51211.html#details-panel5>.
Dault, M., J. Lomas and M. Barer on behalf of the Listening for Direction II partners. 2004. Listening for Direction II: National Consultation on Health Services and Policy Issues for 2004-2007. Retrieved November 21, 2025. <https://www.cda-amc.ca/sites/default/files/pdf/cadth_listening_direction-ll_e.pdf>.
Gagnon, D and M. Menard. 2001. Listening for Direction: A National Consultation on Health Services and Policy Issues. Summary Report (Ottawa: Canadian Health Services Research Foundation, 2001)
Graham, I.D., J. Logan, M.B. Harrison, S.E. Straus, J. Tetroe, W. Caswell et al. 2006. Lost in Knowledge Translation: Time for a Map? Journal of Continuing Education in the Health Professions 26(1): 13–24. doi:10.1002/chp.47.
Institute of Health Services and Policy Research (IHSPR). 2022a, April. Newsletter Spotlight, April 2022. Retrieved January 16, 2026. <https://suivi.lnk01.com/v/443/42688441ee8fe5d211d22b13ccfb066133d8ed93f6f9127f#Spotlight>.
Institute of Health Services and Policy Research (IHSPR). 2022b. Newsletter Spotlight, March 2022. Retrieved January 16, 2026. <https://suivi.lnk01.com/v/443/42688441ee8fe5d25bd9800049d64631c034bfddde0843d3#Spotlight>.
Law, S., C. Flood and D. Gagnon, on behalf of the Listening for Direction III Partners. 2008. Listening for Direction III: National Consultation on Health Services and Policy Issues for 2007-2010. Ottawa, Canada: Canadian Health Services Research Foundation and Canadian Institutes of Health Research, Institute of Health Services and Policy Research. Retrieved January 16, 2026.
Liddy, C., F. McKellips, C. Deri Armstrong, A. Afkham, L. Fraser-Roberts and E. Keely. 2017. Improving Access to Specialists in Remote Communities: A Cross-Sectional Study and Cost Analysis of the Use of eConsult in Nunavut. International Journal of Circumpolar Health 76(1): 1323493. doi:10.1080/22423982.2017.1323493.
Liddy, C., R. Mitchell, S. Guglani, A. Mihan, C. Sethuram, A. Miville et al. 2022. The Provincial Spread and Scale of the Ontario eConsult Service: Evaluation of the First 2 Years. Annals of Family Medicine 20(3): 262–65. doi:10.1370/afm.2812.
McMahon, M., J. Nadigel, E. Thompson, N. Shaid, B. Kasaai and R.H. Glazier. 2022. Accelerating Health System Transformation Through Research to Achieve the Quadruple Aim and Health Equity. HealthcarePapers 20(3): 9–24. doi:10.12927/hcpap.2022.26847.
Morris, Z.S., S. Wooding and J. Grant. 2011. The Answer Is 17 Years, What Is the Question: Understanding Time Lags in Translational Research. Journal of the Royal Society of Medicine 104(12): 510–20. doi:10.1258/jrsm.2011.110180.
Nadigel, J., B. Kasaai, H. Thorsteinsdóttir, S. Rogers, M. McMahon, R.J. Rylett et al. 2025. Research Impact Assessment of a Canadian Digital Health Funding Program: A Case Study. Health Research Policy and Systems 23(1): 81. doi:10.1186/s12961-025-01356-2.
North American Centre for Integrated Care. n.d. Network for Integrated Care Excellence (NICE): A Knowledge Mobilization and Impact Hub for the THINC Initiative. Retrieved January 16, 2026. <https://nacic.dlsph.utoronto.ca/nice/>.
Picard, A. 2023. We Don't Have a Health-Care Crisis, It's an Implementation Crisis, Says André Picard. CBC Radio. Retrieved November 23, 2025. <https://www.cbc.ca/radio/ideas/andr%C3%A9-picard-health-journalism-1.6873829>.
Shahid, N., J. Nadigel, R. Boateng, R.H. Glazier and M. McMahon. 2025. An Evidence-Informed, Community-Engaged Approach to Designing a Large-Scale, Impact-Oriented Research Funding Initiative to Foster the Implementation of Transformative Integrated Care: A Multi-Methods Qualitative Study. Implementation Science Communications 6(1): 86. doi:10.1186/s43058-025-00760-7.
Singer, A., L. Ireland, Z. Sepehri, K. Brown, K. Turner, C. Liddy et al. 2022. Evaluation of BASE eConsult Manitoba: Patient Perspectives on the Use of Electronic Consultation to Improve Access to Specialty Advice in Manitoba. BMC Health Services Research 23(1): 131. doi:10.1186/s12913-022-08913-3.
Wojtak, A. and R. Lewanczuk. 2025. IFIC Canada: Transforming Care Through Integration. Healthcare Quarterly 27(4): 53–58. doi:10.12927/hcq.2025.27581.
Wong, S.T., J.M. Langton, A. Katz, M. Fortin, M. Godwin, M. Green et al. 2019. Promoting Cross-Jurisdictional Primary Health Care Research: Developing a Set of Common Indicators Across 12 Community-Based Primary Health Care Teams in Canada. Primary Health Care Research and Development 20: e7. doi:10.1017/S1463423618000518.
Footnotes
* Co-lead authors
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed